Diabetic foot ulcers are one of the major complications of diabetes. Between 19-34% of all diabetic patients will develop a foot ulcer at some point in their lives 1.
Often underestimated, or even unrecognised by patients, a diabetic foot ulcer can lead to complications such as infection, or in the worst cases, amputation. After amputation, patient life expectancy does not exceed 5 years in 70% of cases, which is lower than the life expectancy for certain types of cancer 2. However, with proper prevention, ulcers can be avoided.
What causes diabetic foot ulcers?
Diabetes does not only cause blood sugar imbalance. It also causes two phenomena which increase the risk of occurrence of a diabetic foot ulcer:
- Involvement of distal nerves in the legs, especially with loss of sensitivity. As a result, patients rarely feel they have an ulcer (neuropathic ulcer).
- Blocked arteries, ultimately leading to insufficient blood flow (ischemic ulcer).
In three out of four cases, diabetic foot ulcers are related to wearing uncomfortable shoes, to an injury caused when cutting the toe nails, to a burn or friction or to fissures and cracks on the soles of the feet.
The longer an ulcer remains open, the more the risk of infection increases. It can lead to amputation in extreme cases.
What is a diabetic foot ulcer?
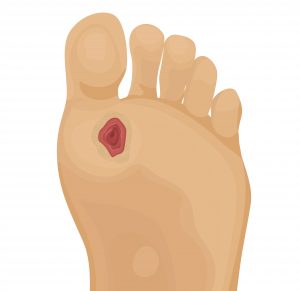 Arising from a minor lesion (caused by anything from a simple cut through to wearing uncomfortable shoes), a diabetic foot ulcer can take three forms:
Arising from a minor lesion (caused by anything from a simple cut through to wearing uncomfortable shoes), a diabetic foot ulcer can take three forms:
- Neuropathic ulcer. Appearing on the toes or under the arch of the foot, as a perforating ulcer of the foot, on the foot joint, this ulcer begins with a callus or corn. It comes with a loss of sensitivity (pain/heat), has clear edges and the skin is dry. In effect, diabetes causes neuropathy which affects the sensory and motor nerves, weakening the extremities of the lower limbs. Therefore the patient’s foot becomes deformed and their nails become curved like claws. The loss of sensation in the foot can even prevent the patient feeling they have an ulcer, which can then rapidly become infected.
- Ischemic ulcer. This is related to a perfusion defect. It mainly occurs on the tips of the toes, on the heel or edge of the foot. The skin breaks, and is pale or bluish in colour. The foot is cold and painful, and the patient can feel burning or itching sensations. Yellow, red, pink, or even black if it is necrotic, the ulcer can take on different colours depending on the stage of progression.
- Neuroischemic ulcer. Linked to neuropathy and associated with ischemia, the ulcer forms on the edge of the foot, tips of the toes, or even under the toenails. The first sign is generally a blister caused by repeated friction of the foot in shoes that are too tight or too narrow.
In adults, an infection is likely to occur in addition to the ulcer, where the wound becomes invaded by bacteria. Diabetic foot ulcers, therefore, mean that diabetes is the leading cause of amputation in the world3.
Diabetic foot ulcer prevention
The Haute Autorité de Santé (HAS)4 has defined a podiatric risk grading system in order to adapt treatment. The foot assessment is used to grade the level of risk according to the following classification:
Grade 0: no sensory neuropathy
Podiatric risk grade 0 means there is no loss of sensitivity in the feet. Standard hygiene rules should be followed, such as wearing appropriate, non-traumatic footwear or avoiding maceration (feet should be dried properly and synthetic socks should be avoided) and traumatic treatments (e.g. use of a scalpel). It is especially important to balance the patients’ diabetes as far as possible and to control any risk factors (e.g.: smoking, arterial hypertension, cholesterol etc.).
Grade 1: isolated sensory neuropathy
In addition to the recommendations that apply for grade 0, you can also follow the advice below for podiatric risk grade 1:
If the ulcer is very painful or uncomfortable, patients should speak to a healthcare professional. Balancing the patients’ blood sugar can provide relief, as can certain medicines.
If the ulcer involves loss of sensation, the patient should inspect their feet daily so that they are able to detect any ulcers that could go unnoticed. It is essential to see a doctor as soon as possible an ulcer is found, even if it is not painful.
It is especially important not to damage the feet by using abrasive or corrosive treatments, by wearing shoes that hurt or walking barefoot. Applying a moisturising cream daily can be beneficial to very dry feet. The patients’ diabetes should be controlled as effectively as possible to prevent the neuropathy worsening.
Grade 2: sensory neuropathy with arteriopathy of the lower limbs and/or foot deformation
These very high risk feet (grade 2 and grade 3) require both increased vigilance on the part of the patient, and active ulcer prevention measures. Podiatrists or nurses can remove the hyperkeratosis (callus). Podiatrists/chiropodists/orthotists can create ortheses or insoles to correct abnormal weight bearing areas. Sometimes, if the foot is very deformed, patients may have to wear specially-made shoes. If there is arterial involvement, revascularisation may be essential.
Treatment
Diabetic foot ulcers require quick and comprehensive treatment to minimise the risk of complications. Regardless of its size, the ulcer must be closely monitored by a multi-disciplinary team.
Wearing a pressure relief device can be beneficial. It means that any weight on the foot will not press on the ulcer, and pressure from walking can be effectively distributed, so as not to aggravate the wound.
Using an appropriate dressing is essential. The dressing should aim to promote healing and should protect the wound and surrounding skin during healing.
The diabetes, comorbidities and nutritional status must also be managed at the same time.
And afterwards?
70% of healed diabetic foot ulcers relapse within 5 years5 . Diabetic patients can help to reduce their risk of relapse by:
- Wearing shoes suited to the shape of the foot, and always with socks
- Never walking barefoot
- Visiting a chiropodist on a regular basis
- Monitoring general foot health (using a mirror to inspect the sole)
- Closely monitoring blood sugar levels and following a diabetes-reducing diet
- Washing their feet daily with soap and water, not forgetting to dry between the toes and using a moisturiser to keep them supple
- Avoiding the use of hot water bottles or similar to warm their feet
